How A PEST Can Help With Psoriatic Arthritis
I looked at the intake form and felt a bit confused.
Back in college, we had weekly sessions that were called an “inreach” where we would treat people with very specific conditions.
Everything from Parkinsons to Multiple Sclerosis.
But this day, the intake form threw me off a bit.
“Psoriatic Arthritis”, but I thought Psoriasis was a skin condition, how did it become arthritis?
I wasn’t sure what to expect but the patient did a great job of explaining what happens with the condition and how massage therapy helped.
But I still didn’t get how a skin condition could become arthritis.
Psoriasis, The Connection To Arthritis And Assessment
The big connection between Psoriasis and Arthritis is inflammation.
In both instances the immune system is attacking the body (skin with psoriasis and joints with psoriatic arthritis) and can have active and remission stages.
But the two are not always linked to each other.
There are instances where the arthritis can set in long before the skin plaques do and vice-versa, about 80% of the time the skin disorder will come first. The arthritis may affect 6-42% of the people who have Psoriasis.
However there is an argument being made in regard to genetic studies saying the two diseases could be separate entities.(1)
Little did I know until researching for this post, there is actually five different types of Psoriatic Arthritis:
- Symmetric – on the same joints on both sides of the body.
- Asymmetric – can affect any joint.
- Distal Interphalangeal Predominant – affects the fingers and toes, close to the nail.
- Arthritis Mutilans – severe and deforming, affects the hands and feet, can also cause neck and lower back pain.
- Spondylitis – affects the spine.
Because patients can present with back pain, we have a real opportunity to help someone in the early stages of Psoriatic Arthritis. It is our job to try an interpret the difference between mechanical or inflammatory back pain.
Inflammatory back pain is chronic (lasts more than three months), so if we have a patient come in this is one of the red flags we can look at during our assessment to dig a little deeper and see what’s happening.
Fortunately people way smarter than me have come up with a way to figure this out!
It’s called the PEST tool (Psoriasis Epidemiology Screen Tool) and you can download what a copy looks like here.
It is recommended that anyone with Psoriasis gets tested once a year to see if they have developed Psoriatic Arthritis.
The PEST tool is a series of five questions:
- Have you ever had a swollen joint?
- Has a doctor ever told you that you have arthritis?
- Do your fingernails or toenails have holes or pits?
- Have you had pain in your heels?
- Have you had a finger or toe that was completely swollen and painful for no apparent reason?
They are given a score of 1 for each question they answer yes to, anything over a score of 3 can indicate the arthritis.
The patient is also given a picture of the body and told to circle any joints where they have felt discomfort.
Although those five questions can help to determine there is a problem, it doesn’t help as far as someone with inflammatory back pain.
So there are a few extra questions you can ask:
- Do you experience early morning stiffness that lasts more than 30 minutes?
- Have you had neck or back pain for more than 3 months?
- Does the pain wake you up early morning?
- Does it get better after exercise or movement?
Now of course we CANNOT diagnose any of this, but it is good information to know as part of our assessment, especially if we are seeing any patients who have Psoriasis.
If you decide to use the PEST tool and it raises some concerns, always make sure to refer the patient back to their doctor or a rheumatologist.

Photo by: stevepb
Treating Psoriatic Arthritis
It was a little tough (well for me it was at least) to find a lot of research involving massage therapy and specifically Psoriatic Arthritis, there’s plenty around the other various types of arthritis though.
Generally most of what I could find revolved around moderate pressure massage and the beneficial outcomes of this style of treatment.
We obviously don’t want to use deeper pressure techniques on a person dealing with an inflammatory disease as it would only make things worse.
Not surprisingly a number of articles also focused on the psychological benefits associated with treatment and also around educating the patient in conjunction with treatment.
With all we’ve been learning on pain science it makes sense that education and associated benefits with the psychological side of things would have a benefit to the patient with the pain associated with any one of the different types of arthritis.
One study talks about the toll fatigue has on patients dealing with Psoriatic Arthritis and how recommendations on sleep hygiene, exercise, goal setting, stress reduction and relaxation as a major benefit in coping with the disease. (2)
We all know how great a job massage therapy does of helping people relax!
Most of the other studies I found fell under the umbrella of physical therapy and it’s benefits (3) to helping with various forms of arthritis (yes there were more than the one I just cited, but most were saying the same thing), with movement being one of the bigger contributing factors. But one study specifically looked at the benefit of using joint mobs and exercise in treating carpometacarpal joint osteoarthritis and showed it beneficial in treating pain.(4) In most cases it is clear that more research is needed on the topic. Keeping in mind the contraindication of treating anyone who is experiencing a flare up with their arthritis, massage therapy can be beneficial in helping to treat this. Throw in some joint mobilizations with some active and passive range of motion and you’ll probably look like a rock star in helping out that patients that come in. Use the PEST tool as part of your assessment if you or your patient aren’t sure whether arthritis is setting in and it can go a long way, not only in understanding what’s going on but also their quality of life. But most of all hopefully you don’t have to get your patient to explain everything to you like I did!
References
- Boehncke W. Psoriasis and Psoriatic Arthritis: Flip Sides of the Coin?. Acta Dermato-Venereologica [serial on the Internet]. (2016, May), [cited October 3, 2016]; 96(4): 436-441. Available from: MEDLINE with Full Text.
-
Waldron N. Care and support of patients with psoriatic arthritis. Nursing Standard [serial on the Internet]. (2012, Aug 29), [cited October 3, 2016]; 26(52): 35-39. Available from: CINAHL Complete.
-
Vlak T. [Spondyloarthropathies–clinical evaluation and physical therapy]. Reumatizam [serial on the Internet]. (2004), [cited October 3, 2016]; 51(2): 29-33. Available from: MEDLINE with Full Text.
- VILLAFAÑE J, CLELAND J, FERNÁNDEZ-DE-LAS-PEÑAS C. The Effectiveness of a Manual Therapy and Exercise Protocol in Patients With Thumb Carpometacarpal Osteoarthritis: A Randomized Controlled Trial. Journal Of Orthopaedic & Sports Physical Therapy [serial on the Internet]. (2013, Apr), [cited October 3, 2016]; 43(4): 204-213. Available from: SPORTDiscus with Full Text.
- Episode #29 Dealing With Burnout - May 25, 2026
- Episode #28 With Great Educational Power, Comes Great Educational Responsibility - May 25, 2026
- Episode #27 Myofascial Release And CLB, What Does The Evidence Say? - May 25, 2026
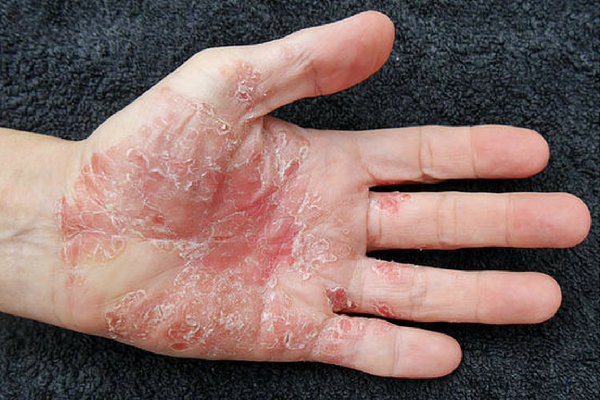



I developed guttate psoriasis approximately 5 years ago, after seeing 2 skin specialists with reasonable results. About June last year it flared up into something awful on my legs, arms, hands, buttocks, back and scalp. I gave up my job as it involved contact with the public and off I went to another dermatologist. He just asked a few questions, had a look at the affected areas and immediately arranged for phototherapy treatment at the local hospital. What magic! After 21 sessions which ended on a 2 minute treatment, 95% of lesions disappeared. Now I just use Daivobet cream for body and gel for scalp when it looks like something maybe forming. I shampoo and condition with T-Gel alternating days with goat milk hair products. Needless to say, I am much happier these days.
It’s interesting that anything over a score of 3 means that they might have arthritis. My dad would probably answer yes to most of those questions. I’ll have to get him to see a doctor for treatment soon.