Motivational Interviewing In Your Clinic
A great deal of our work as therapists involves helping people to make changes in order to get better outcomes, be it for general health and well-being, reductions in pain, or increases in mobility.
Our training and education means that we know a lot about what people need to do to achieve these outcomes. We are smart and we know it! We assume the patients coming in to see us, know that too. So it should be simple right, we tell them all the things that they need to know, and they go away and do it. But here lies the problem, no one really wants to be told what to do.
Take for example the person who has recently had a heart attack but is also a smoker. They are very likely to be informed of the fact that continuing to smoke is going to contribute to poor health outcomes including increasing the risk of another heart attack. With such a frightening near death experience, one might assume that being given sufficient information, combined with the fear of the experience would be enough to make someone stop smoking.
However the studies tend to tell us that only about half the people in this situation will actually quit smoking! (1) Mind blowing isn’t it? What this and many other studies in similar fields of healthcare continue to show us is that information and fear are not enough to change behaviour, no matter how dire the consequences. (2)
Changing Our Approach For Better Outcomes
Self management forms a big part of the picture in managing all chronic diseases. As we start to view pain with a more modern and science based understanding, our approach to treating it should start to shift away from trying to “fix” the patient and towards an empowering model of care that encourages the patient to take their health into their own hands.
Sounds easy doesn’t it?, but many of us have been experiencing as practitioners what an uphill battle this is. Particularly in our western culture where there is an understanding around medicine being able to “fix” everything, so that the mere presence of pain is viewed as being “wrong”, and the understanding that as a consumer based system, you just have to pay for the “thing” (manual therapy/ acupuncture/ surgery/ injections etc) and it will be done to you and will be effective.
Unfortunately, we know it doesn’t work like that.
Single modality approaches for treating any pain condition, but particularly chronic pain, are largely unhelpful in the long term and science tells us that adopting an active approach is far more likely to lead us to better outcomes. (3)
In treating pain and getting people to adopt behavioral change, some of the information we provide to help, might be of a therapeutic neuroscience education (TNE), explaining pain, pain education approach. Along the lines of what we see in situations like smoking cessation, weight loss and exercise programs, providing the information doesn’t always translate through to the outcomes we might hope.
That is not to say that we don’t use it.
The research tells us it has value (4-7) , we just understand that it is one part of the process, the information and context a person might use when deciding on taking a multidisciplinary and active approach to treating their pain.
Motivational Interviewing
Motivational interviewing is a cognitive behavioral technique that helps patients to identify behaviors that may be preventing them from achieving optimal management of a chronic condition. It has been used in many healthcare settings which require behavioral change for better outcomes such as addiction medicine, oral-health self care, smoking cessation, weight loss, medication compliance and diabetes self management. It identifies a cycle that people tend to go through (and often go back around and around) in processing a change in behaviour.(2)
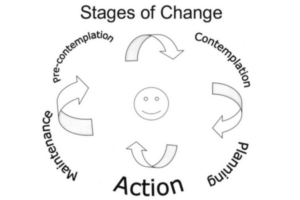
The process of motivational interviewing is one that provides structure around helping a person to find their own motivation, the idea being that if a person has made the choice for themselves they are far more likely to follow through with change, compared to when it is something that has been forced upon them.
It is a process that requires first establishing a level of rapport with the person and then helping them to identify what behaviors they would like to change. Within the approach there are some specific techniques that can help the practitioner to elicit in the patient a better understanding of what his or her thought processes are in relation to the problem. Then through a process of reflective listening and open ended style questioning, helping the person to identify how important the change is to them and how confident they are in being able to make those changes. From there a structured, but collaborative approach can address the barriers to change, identify measures of support and create a plan to move forward that fits with the patient’s own motivation.
The best thing about motivational interviewing is its accessibility. It is a process that has been used in industries other than just psychology, (sales and human resources to name a few). This means that it is easy to learn about it and that applying it in the clinic is not an “all or nothing principle”.
You can start to learn about some of the elements and apply them straight away – the easiest way is to refine your listening and reflecting skills and resist the urge to jump in straight away and tell people what they “should” be doing. There are lots of resources available in the form of short courses, blog post summaries, books and journal articles. So if you are feeling motivated, get your google on and work out what your next best step is to start delving into some motivation interviewing skills! (2)
References:
1. van Berkel TF, van der Vlugt MJ, Boersma H. Characteristics of smokers and long-term changes in smoking behavior in consecutive patients with myocardial infarction. Prev Med 2000, Dec;31(6):732-41.
2. Bundy C. Changing behaviour: Using motivational interviewing techniques. J R Soc Med 2004;97 Suppl 44:43-7.
3. O’Keeffe M, Purtill H, Kennedy N, Conneely M, Hurley J, O’Sullivan P, et al. Comparative effectiveness of conservative interventions for nonspecific chronic spinal pain: Physical, behavioral/psychologically informed, or combined? A systematic review and meta-analysis. J Pain 2016, Jul;17(7):755-74.
4. Louw A, Diener I, Butler DS, Puentedura EJ. The effect of neuroscience education on pain, disability, anxiety, and stress in chronic musculoskeletal pain. Arch Phys Med Rehabil 2011, Dec;92(12):2041-56.
5. George SZ, Childs JD, Teyhen DS, Wu SS, Wright AC, Dugan JL, Robinson ME. Brief psychosocial education, not core stabilization, reduced incidence of low back pain: Results from the prevention of low back pain in the military (POLM) cluster randomized trial. BMC Med 2011;9:128.
6. Van Oosterwijck J, Meeus M, Paul L, De Schryver M, Pascal A, Lambrecht L, Nijs J. Pain physiology education improves health status and endogenous pain inhibition in fibromyalgia: A double-blind randomized controlled trial. Clin J Pain 2013, Oct;29(10):873-82.
7. Moseley GL. Evidence for a direct relationship between cognitive and physical change during an education intervention in people with chronic low back pain. European Journal of Pain 2004, Feb;8(1):39-45.
- Motivational Interviewing In Your Clinic - March 6, 2017



