Managing A Collapse In Your Massage Therapy Clinic
Like it or not, it is going to happen one day.
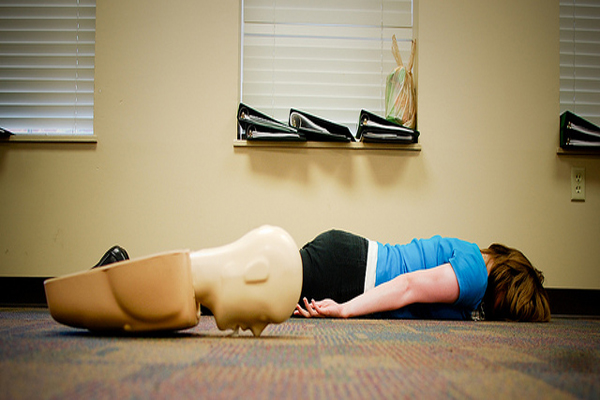
You do your intake with a patient, leave the room and on your return there they are, lying on the floor not breathing.
Your adrenaline rushes because you never thought you’d actually have to deal with this…ever.
But the odds are against you.
According to the heart rhythm society, in the U.S. more than 350,000 deaths occur each year because of sudden cardiac arrest, which is more than breast cancer, lung cancer or AIDS.
Sudden cardiac arrest takes an average of one life every two minutes.
Unfortunately 95% of people who suffer a cardiac arrest lose their life because of delayed treatment.
However the bright side is that you can help. The odds of being able to revive someone greatly increases when you witness the collapse.
Fortunately when we have our patients in the clinic, chances are we are going to witness the collapse in case they experience a cardiac arrest.
Initial CPR
If you ever witness a collapse, or walk back into your massage treatment room and see someone unconscious, the first thing you have to do is assess if the person is breathing.
We do this by using a technique called: “look, listen and feel”.
Firstly, squeeze the persons traps and see if they respond in anyway. Then put your ear overtop the persons mouth, place a hand on their chest and look at the chest for 15 seconds.
See if you can feel a breath on your ear and watch to see if your hand on the chest rises at all to indicate breathing.
If there is no air exchange occurring, tilt the persons head back, check to see if they start breathing. If they don’t start breathing on their own keep the head tilted back and attempt to give the person two breaths.
Watch to see if the chest rises, indicating air going into the lungs.
If the chest rises, it shows that the person has an open airway, so you can begin chest compressions (if the air didn’t go in, it means something is blocking the airway so they could have choked on something).
If they had choked on something, you would start compressions as well, however the intent of the compressions now is to clear whatever the person had choked on.
To start your compressions, landmark at the persons armpit on the side of the body opposite to you. Then bring the palm of your hand up to the sternum and deliver 30 chest compressions.
Continue to deliver 30 compressions and two breaths until more help arrives.
Once you realized the person was not breathing and CPR was necessary it is important to get someone to call 911 for you, and if available get an A.E.D. (automated external defibrillator).
If you’re on your own, grab a phone, bring it back to the person and call 911. Put it on speaker phone and the 911 dispatchers will coach you on what to do.
Using An AED
People often think that an AED works like the paddles the doctors on TV shows like ER use to jumpstart a persons heart.
It doesn’t work like that.
If the heart is completely stopped and flat lined, the AED isn’t going to do anything.
There has to be a “shockable” rhythm, a tachycardia (fast rhythym) or bradycardia (slow rhythym) for the AED to do anything.
There are a few things to take into consideration when using an AED.
If you are in a wet environment (you sports therapists) you have to do a splash test.
If the ground is wet and you slap it, if it makes a splash you have to move the person before you can allow the AED to deliver a shock. If the ground is just wet and there is no splash, it’s fine to deliver the shock.
If the person has a really hairy chest, then you have to shave the chest before putting the pads on. The pads have to be in direct contact with the skin to work properly (fortunately AED kits come with a razor in them).
Also if there is any metal (ie: underwire bra, jewelery etc.) in the path of the pads, it should be removed or it will leave burn marks. Same for any kind of nicotine or medical patches, they should come off.
Then just turn the machine on and follow the directions, don’t try and jump ahead, just do what it tells you.
Make sure when the machine says “everyone stand clear”, no one is touching the patient. If someone was still doing compressions, the machine would read that as the rhythm of the heart instead of it’s actual rhythm.
Also, the second time it advises to make sure “everyone stand clear”, is when it’s about to deliver a shock. Make sure no one is touching the patient or they will get shocked as well.
If the AED detects a “shockable” rhythm it will deliver a shock and you will see the body rise up a bit.
If there is not a “shockable”rhythm it will say: “no shock advised, continue doing two minutes of CPR”.
If you have a second person with you, have them take over doing CPR, so you get a break. Then alternate with the other person every two minutes so that one person doesn’t get tired out.
It should look something like this:
This can be a pretty scary situation to have to deal with. I honestly hope you never have to. However if this ever happens and the outcome isn’t what you had hoped for, please reach out and talk to someone about it. As healthcare professionals we are constantly telling patients to do proper home care, or are referring people to get more help should they need it. This is one of those cases where we really have to take care of ourselves after an incident like this. Chances are if this happens in your clinic, you already have a therapeutic relationship (and possibly a long standing one) with your patient. Going through a shocking scenario (no pun intended) such as this can bring up some very strong and sometimes scary emotions from the person who has to perform CPR. So please reach out and get some counselling or talk to some sort of mental health professional should you ever go through this. Remember how important your own self care is.
- Podcast Episode #29: Dealing With Burnout - April 11, 2023
- Podcast Episode #28 With Great Educational Power, Comes Great Educational Responsibility - November 8, 2022
- Podcast Episode #27 Myofascial Release And CLB, What Does The Evidence Say? - August 30, 2022








Amazing post for anyone that works with … anyone! I haven’t taken CPR or any first aid and should – this reminded me of the importance of knowing the basics. Of course I also love that you recommend seeing a professional to do with the trauma of having someone collapse and vicarious trauma that health care professionals experience in their careers in general. Solid post with huge value massage therapists and anyone else!
Very valuable information. It’s great to see RMTs maintain such high standards for their profession.
There are never too many articles about CPR. I don’t know CPR, but the more I read and understand its practicality… well, I need to learn.