How A Massage Therapist Can Handle An Allergic Reaction
The scary thing is, you never know how severe an allergic reaction is going to be.
When I showed up, I couldn’t believe the state she was in.
Mere steps away from the medication that could have saved her life, but she just didn’t get to it in time.
We cycled through CPR for 45 minutes but our efforts were in vain. We couldn’t bring her back.
It’s an issue everywhere these days.
Allergic reactions to so many foods, substances and insects. Such innocent things but enough for a person to lose their life.
At any given moment we could see this in our clinic, at an outreach or just in day-to-day life.
The Signs and Symptoms You Need to Know
People who have this type of severe allergy (anaphylaxis) generally know they have it and will let you know if you need to deal with it.
There are a few different things that can cause anaphylaxis, the most common being food allergies and insect stings. Reactions can also be brought on with latex allergies, participating in exercise, medications and sometimes for no reason at all.
May is food allergy awareness month and if you’ve never seen someone having this kind of reaction, the Red Cross First Aid & CPR Manual highlights some signs to look for.
They may end up with:
- Hives
- Itching
- Rash
- Weakness
- Nausea
- Vomiting
- Dizziness and
- Breathing Difficulties
You may remember the Big Bang Theory episode where Wolowitz ate the granola bar to get Leonard out of the house?
Although it doesn’t look that extreme in real life, it gives you a bit of an idea what is happening when a person has a reaction.
If left too long the reaction can have dire consequences. In the story I told at the beginning, the person was ten feet from their medication which was the difference between life and death. These allergies are so common now that schools are limiting whether kids can bring peanut butter sandwiches or other peanut ingredient snacks to school.
There has even been huge arguments over whether it is okay to use one student’s medication on another student having a reaction, to the point that schools are now having to carry their own supplies in case of emergency.
What Can Massage Therapists Do To Help?
Our biggest responsibility is to help the person breathe, so getting them sat down in a position of comfort to make breathing easier is the first step. This is usually going to be in a seated position leaning forward so that it takes some pressure off the diaphragm.
There are so many stories out there about how people panic when this type of thing happens.
They do their best to help but then get flustered. Time is of the essence here, the person needs that medication and they need it NOW.
Slow down, breathe and don’t panic. If the person sees you worked up it’s only going to cause them further stress that will worsen their condition.
The next step is to get that felt pen looking thing. It’s called an EpiPen and contains the hormone epinephrine.
Once delivered the epinephrine should start to relieve the swelling in a person’s airway and make breathing easier. But before they take the shot of medication there are a couple of things you should check.
- Make sure it is their EpiPen
- This is important if it is not with them and you have to go get it. Always make sure you are giving a person THEIR medication with THEIR specified dose.
- Ask them “is this yours?” and hold it up in front of them to confirm it.
- Check the expiry date.
- If the medication is expired it should not be used (unless it’s your only option as a last resort), which means that calling 9-1-1 is a good idea at this point as the Ambulance will have medication with them.
Fortunately the design on new EpiPen’s are a lot easier to use than the older style ones and cause a lot less confusion.
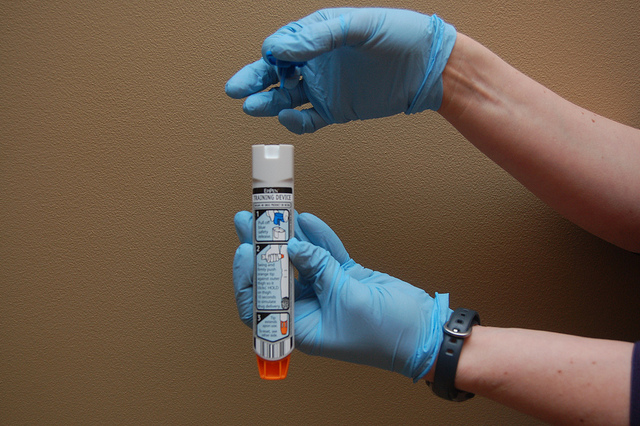
If you’ve never seen or used one before they’re pretty simple to use. One end is blue and the other end is orange. The orange end is where the needle comes out to deliver the medication, so don’t get the two mixed up (you don’t want to have a person stick the needle into their thumb). All you have to do is get the pen out of the case and it’s ready to go.
- Pop the cap on the case and remove the EpiPen.
- Remove the blue cap at the top of the pen.
- The patient plunges the orange end into their thigh and holds for around 10 seconds.
- Monitor the person’s ABCs to make sure the medication is working.
It shouldn’t take too long for the person to start feeling the effects and make breathing a little easier. However they should still seek medical attention because sometimes the epinephrine can start to wear off, making breathing difficult again.
Remember that we cannot deliver the medication, the patient has to do it themselves.
Make sure to call 9-1-1 after to make sure they get needed medical attention.
Do not leave the person alone while you wait for paramedics to arrive. Your responsibility now shifts to making sure their ABCs are maintained in case their airway starts to swell.
As healthcare professionals you can contact www.epipen.ca and there is a wealth of information on the site about how to use an EpiPen, allergic risk factors, video tutorials and they will even send you an EpiPen training device for practice.
I always assumed you had to have a prescription to get an EpiPen but I contacted Anaphylaxis Canada and they informed me you can get them behind the counter in all pharmacies in Canada (however in the U.S. it is still obtained by prescription only). If you’re doing much treatment outdoor, on site or even if you’re just worried about some of your patients in clinic, for the cost of around $85 it might be a good investment for your practice.
If you decide to keep some with you or in your clinic, make sure you only give it to someone who has used it before and has had it prescribed by their doctor.
At least (if nothing else) Howard Wolowitz has taught us what an allergic reaction could look like, and maybe how not to be too creepy.
- Episode #29 Dealing With Burnout - May 25, 2026
- Episode #28 With Great Educational Power, Comes Great Educational Responsibility - May 25, 2026
- Episode #27 Myofascial Release And CLB, What Does The Evidence Say? - May 25, 2026




Hi Jamie,
Thank you for posting your article, It is interesting !
Keep posting !
No problem, glad you enjoyed it. Thanks for reading.
I didn’t know that massage therapists could help with saving someone from an allergic reaction. I think it would be smart to have some of these EpiPens around so that you can help. The therapists should be able to help when trouble like this happens.
Hey Charles, well you should take a proper first aid course in order to know how to help properly. I think it’s one of the most valuable courses a Massage Therapist can have because you never know when something could happen in your clinic. Thanks for commenting.
I knew massage therapists can do a lot of things, but I had no idea that they could help people breathe calmly in the case of anaphylaxis! Along with discussing how they can help, I am glad you described what to do in the case of an allergic reaction. I hope no one has to see one in person!
Thanks Luke, glad you enjoyed the post. Hopefully no one has to deal with it, but now hopefully they’re a little more prepared just in case!
That’s a great piece of information. I didn’t know that a massage therapist can save you from an allergic reaction. This would be very helpful for those living away from cities and lack proper facilities like hospitals etc.
Thank you, Jamie.
Well it’s not necessarily that a massage therapist could save someone from an allergic reaction, but rather anyone with first aid training should be able to help someone going through this. Thanks for reading Sarah, glad you enjoyed it.